Upfront Risk-Free Pricing
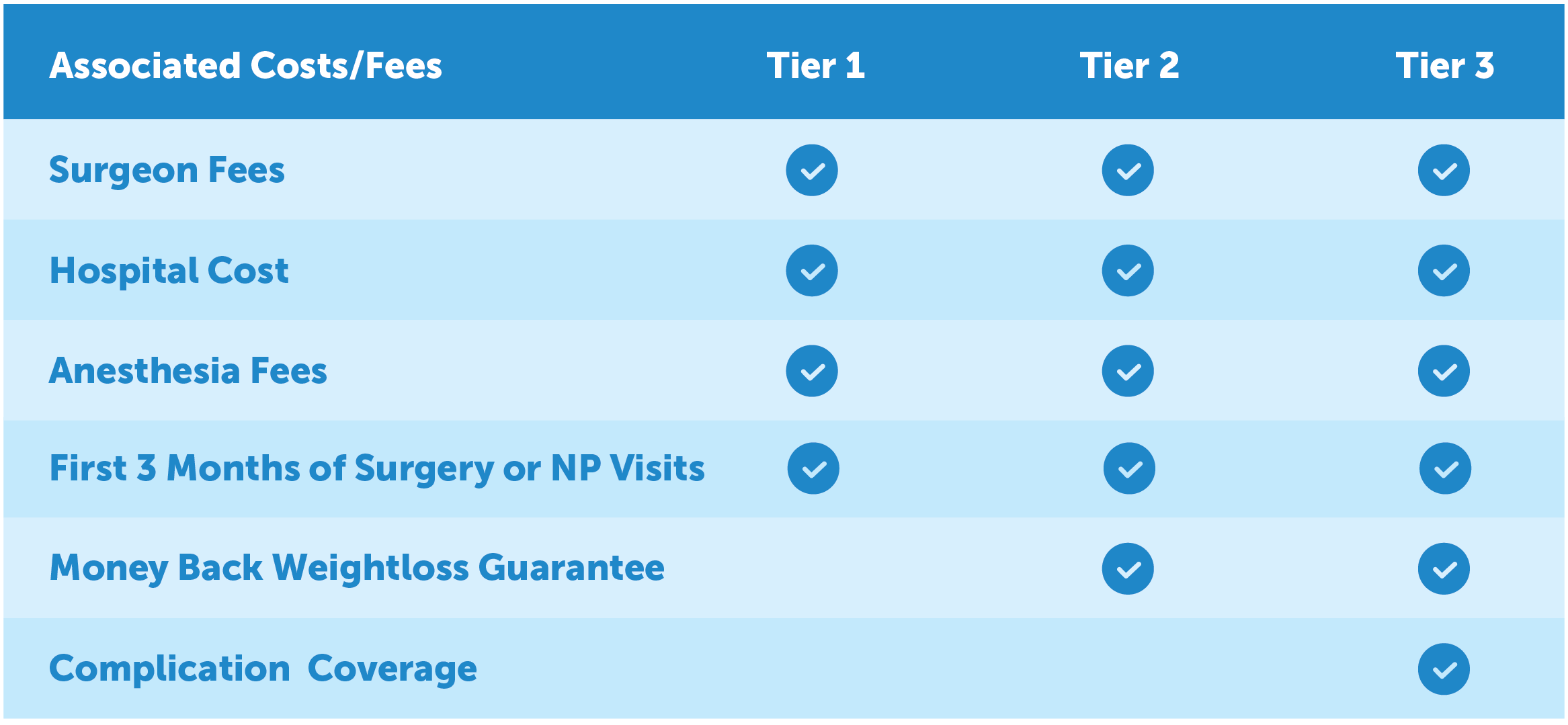
This new three-tiered pricing system guarantees transparency, ensuring that our patients know what their costs will be upfront.
Tier 1
Sleeve – $9,995
Roux-n-Y – $15,000
Duodenal Switch – $15,000
Tier 2
– Surgery + Money back weight loss
guarantee
Sleeve – $11,995
Roux-n-Y – $17,000
Duodenal Switch – 17,700
Tier 3
– Surgery + Money back weight loss
guarantee + Complication insurance through BLIS
Sleeve – $13,165
Roux-n-Y – $18,608
Duodenal Switch – $18,878
*Individual insurance plans may have additional costs associated with treatment. Speak with your insurance provider for details.
For more financial scenarios, please look at Financial Questions
Financial FAQs
WeightWise strives to make Bariatric Surgery as affordable and accessible as possible. Unfortunately, many insurance plans offer limited to no coverage for the various procedures. We know that many patients’ top concern is paying for their surgery and while we can’t answer every specific question, we hope the information below will provide a general overview of the various financing arrangements typically found at WeightWise.
There are three financing situations we generally encounter:
- Situation #1: No Health Insurance Coverage (cash pay)
- Situation #2: Have Health Insurance, No Bariatric Surgery Benefits
- Situation #3: Have Health Insurance and Bariatric Surgery Benefits
Situation #1: No Health Insurance Coverage (cash pay)
The prompt pay discounted prices (pre-pay) below reflect uncomplicated hospital stays.
- Laparoscopic Adjustable Gastric Band (LAGB)- $8,995
- Laparoscopic Roux-en-Y Gastric Bypass (LRnYGB) – $15,000
- $5,000 surgeon fees
- $1,200 anesthesia
- $8,800 hospital fees
- Laparoscopic Gastric Sleeve (LGS) – $9,995
- $3,700 surgeon fees
- $900 anesthesia
- $5,395 hospital fees
- Single Anastamosis Duodenal Switch – $15,000
- $5,000 surgeon fees
- $1,200 anesthesia
- $8,800 hospital fees
- Revisional SADS – $13,000
- Obalon Balloon – $7,500
The above prices cover the surgeon, assistant surgeon, anesthesia and an uncomplicated hospital stay. There will be additional charges for pre-operative services, additional procedures (such as an EKG, sleep study, etc.) and pre-payment of post-operative services. More information about these charges will be available at the informational seminar.
Situation #2: Health Care Insurance Coverage, but No Bariatric Surgery Benefits
We make every effort to verify health insurance benefits before the initial consultation. If no bariatric surgery benefits exist, the prompt pay rates for their actual surgical event apply (see above – Situation #1). Additional procedures such as EKG, sleep study and lab work are often covered by these policies.
For all covered visits, the patient should expect to pay the “specialist” co-pay specified by their insurance plan.
Situation #3: Have Health Insurance and Bariatric Surgery Benefits
We make every effort to verify health insurance benefits before the initial consultation. After your consultation we will also follow up with your insurance company with a “Letter of Medical Necessity”. If bariatric surgery benefits exist, the patient will be responsible for applicable co-pays, co-insurance and deducible up to their out-of-pocket max. Additional procedures such as EKG, sleep study and lab work are often covered by these policies.
Coverage for the surgeon’s portion of the procedure is wholly separate and distinct from coverage for services received from the hospital and anesthesia. Inquiries regarding hospital or anesthesia services may be directed to Summit Medical Center Business Office at 405-359-2488, Integris Baptist Medical Center Business Office at 405-951-4740 and OU Medical Center Business Office at 405-271-6892
WeightWise does no internal financing, we recommend the following finance companies below.
Care Credit (800-859-9975, www.carecredit.com)
Allegiance Credit Union (405-789-7900, www.allegiancecu.org)

All this information and more will be covered in the informational seminar. During the initial consult, a patient advocate will be assigned to guide you through the process. If you have questions at any time after the first consult, please contact your patient advocate.
Please feel free to call for a list of insurance plans that we are in network with at 405-359-2475
